Click on the links below to find out more
Hip Dysplasia-Adolescent
DESCRIPTION
In patients with hip dysplasia, the acetabulum is shallow, meaning that the ball, or femoral head, cannot firmly fit into the socket. As a result of this abnormality, there is increased stress on a smaller area of the joint, which can result in pain and early degeneration of the hip. The labrum can end up bearing the forces that should normally be distributed evenly throughout the hip joint. In addition, more force is placed on a smaller surface of the hip cartilage and labrum. Over time, the smooth articular cartilage becomes frayed and wears away and the labrum becomes torn or damaged. These degenerative changes can progress to osteoarthritis.
HIP DYSPLASIA
The magnitude and severity of hip dysplasia can vary from patient to patient. In mild cases, the head of the femur may simply be loose in the socket. In more severe cases, there may be complete instability in the joint and/or the femoral head may be completely dislocated out of the socket.
A slippery tissue called articular cartilage covers the surface of the ball and the socket. It creates a smooth, low friction surface that helps the bones glide easily across each other.
The hip is one of the body’s largest joints. It is a “ball-and-socket” joint. The socket is formed by the acetabulum, which is a part of the large pelvic bone. The bone surfaces of the ball and socket are covered with articular cartilage, a smooth, slippery substance that protects and cushions the bones and enables them to move easily.
Cause
Adolescent hip dysplasia usually results from developmental dysplasia of the hip (DDH) that is undiscovered or untreated during infancy or early childhood.
DDH tends to run in families. It can be present in either hip and in any individual. It usually affects the left hip and occurs more often in:
- Girls
- First-born children
- Babies born in the breech position
Symptoms
Hip dysplasia, itself, is not a painful condition. However, pain results when the altered forces in the hip cause degenerative changes to occur in the articular cartilage and the labrum. In most cases, this pain is:
- Located in the groin area, although it may sometimes be more toward the outside of the hip
- Occasional and mild initially, but may increase in frequency and intensity over time
- Worse with activity or near the end of the day
- Some patients may also experience the feeling of locking, catching, or popping within the groin.
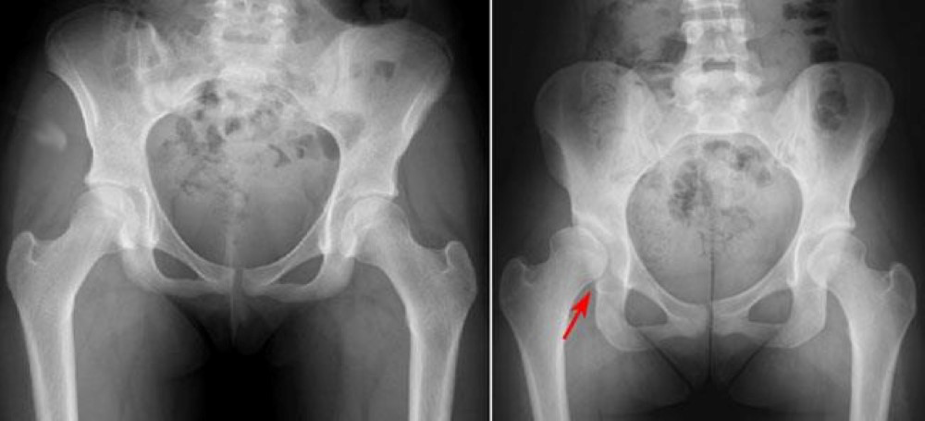
(Left) This x-ray shows two normal hips. (Right) The red arrow shows a dysplastic hip. The hip socket is shallow and there is only partial coverage of the femoral head (ball).
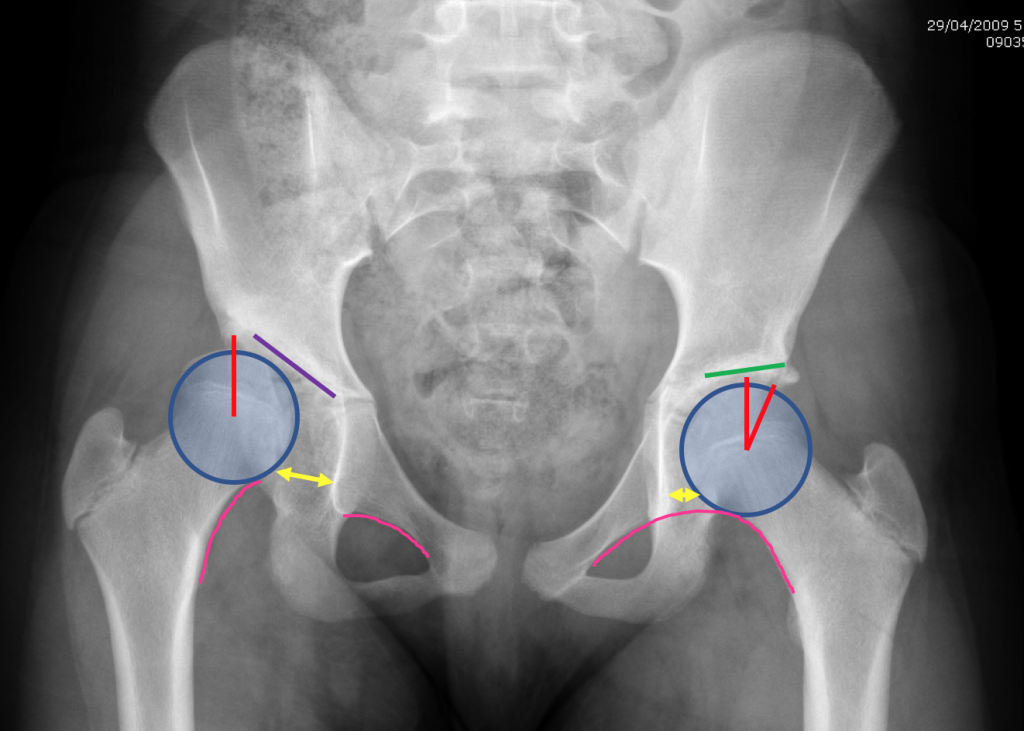
(Left) Dysplastic Hip. Lines on X Ray to indicate Hip Dysplasia: Sloping Roof – note the difference between the purple and green lines; Joint dislocation: note increased size of the space on the left indicated by the yellow arrow and the break in the pink line; reduced coverage of the femoral head on the left side indicated by the red line compared to the right side.

As the hip slides in and out of joint the cartilage wears out – similar to the tyres on a car which is out of alignment
Imaging
In most cases, adolescent hip dysplasia can be diagnosed with x-rays.
X-Rays
These provide images of dense structures such as bone, and will help assess the alignment of the acetabulum and femoral head. An x-ray can also show signs of arthritis.
Computed tomography (CT) scans
More detailed than a plain x-ray, CT scans can help establish the degree of dysplasia and overall shape of your hip. They are also important at assessing the direction that the hip socket is facing (forwards – anteversion, or backwards – retroversion). They are also very useful for looking at the femur (thighbone) and how it is aligned.
Magnetic resonance imaging (MRI) scans
These studies can create better images of the body’s soft tissues. An MRI helps define the integrity of the labrum and articular cartilage. Dr Slattery routines uses advanced imaging techniques of DGEMRIC and cartilage mapping sequences, which are only provided at certain radiology practices. These are very useful for determining the success of hip preserving surgery pre-operatively.
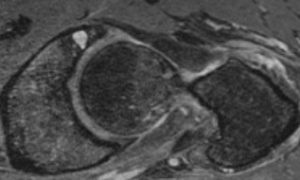
Above: Normal MRI shows possible cartilage damage
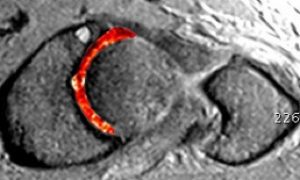
Above: dGEMRIC MRI shows cartilage damage

Dr David Slattery
FRACS MBBS (Hons) LLB FAOrthA
Dr David Slattery is an orthopaedic surgeon based in Melbourne with over 10 years of experience, with a special focus on hip and knee joint preservation and replacement. With qualifications in both medicine and law, he brings a unique and comprehensive approach to patient care. His surgical techniques are minimally invasive and evidence-based, designed to reduce pain and enhance recovery.
Trained in leading institutions across Europe and the USA, Dr Slattery offers advanced treatments for a wide range of joint conditions. He is deeply committed to patient outcomes and takes pride in tailoring treatment plans to each individual. Whether you’re an athlete or seeking relief from chronic joint pain, his goal is to restore function and improve your quality of life.